How Texas Insurers Verify Pre-Existing Injuries After a Car Accident
Every article on this site is researched by our internal team, reviewed for legal accuracy against current Texas law, and held to State Bar of Texas advertising standards before publication. We do not publish content that overstates outcomes or makes promises about results.
Learn more about our
editorial standards .
Key Takeaways
- Insurers verify pre-existing injuries through medical records, imaging comparisons, prior claims, recorded statements, and independent exams.
- Under Texas law, you can recover for an aggravated pre-existing condition if evidence shows the crash worsened your baseline function.
- Building a strong proof package with timelines, baseline documentation, and treating physician notes is essential to counter insurer arguments.

How Texas Insurers Verify Pre-Existing Injuries After a Car Accident
You were rear-ended in rush hour traffic on Alameda Avenue in El Paso last month. Your neck and back hurt worse than they have in years. The problem is you had back surgery three years ago, and now the insurance adjuster keeps asking about your “prior condition.” You’re worried they’ll use your medical history to deny your claim entirely.
This concern is valid. Insurers routinely investigate pre-existing conditions to minimize payouts. Understanding how they verify these injuries and what you can do to protect your claim makes a real difference in Texas personal injury cases.
Pre-Existing Conditions vs. Aggravations vs. New Injuries
Texas injury claims can hinge on whether the crash aggravated a prior condition, caused a completely new injury, or caused no compensable change at all.
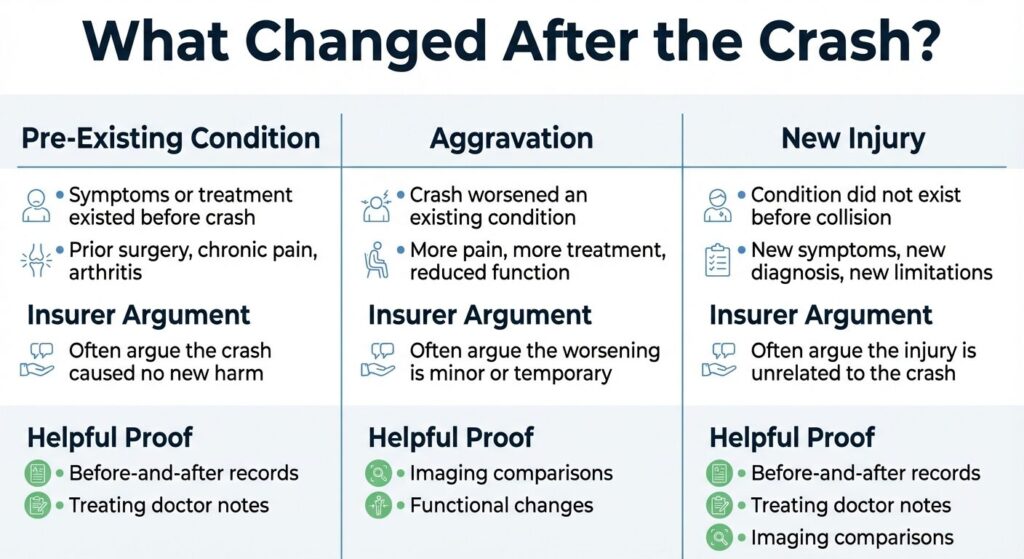
Per 28 Tex. Admin. Code § 3.3018, pre-existing condition is generally understood in insurance terms to be a condition which either already had existing symptoms or that you were previously treated for before the incident. This could be a prior surgery, chronic pain, arthritis, or degenerative disc disease. Insurers focus less on diagnostic labels and more on your symptoms and function before the crash.
In a car accident claim, the more important question is whether the crash caused a new injury or whether it aggravated that prior condition.
Aggravation means the crash in question made a pre-existing condition worse by re-injuring the impacted body part. This could mean increased pain levels, new physical limitations, additional treatment needs, or a measurable decline in function. For example, if you had occasional back pain before but now can’t work or sleep due to pain severity, that’s aggravation.
Texas courts treat causation as the key issue, which is why insurers dig into your prior records and why clear before-and-after medical documentation can make a major difference.
Texas follows the eggshell skull rule. This legal principle means you don’t have to be perfectly healthy to have a valid claim. If a crash causes greater harm because of a pre-existing vulnerability, the at-fault driver is still responsible for all resulting damages. This is often the reason why insurers try to push back against aggravations as hard as they do.
Verifying a Pre-Existing Injury in Texas
When an insurer “verifies” a pre-existing injury, they’re building a causation argument. They want to show that your current symptoms existed before the crash and that the collision didn’t change anything meaningful.
Insurance companies use multiple sources to build their position on causation. Knowing what they look for helps you prepare.
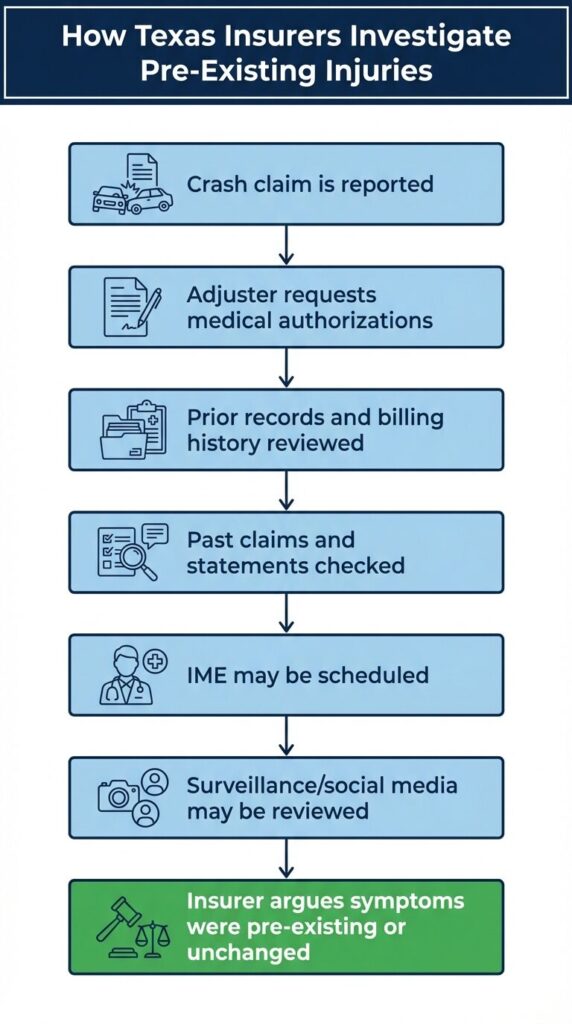
Medical record requests and authorizations are the primary tool. Adjusters review prior complaints, earlier imaging, past referrals to specialists, and treatment patterns. They’re looking for any mention of the same body part or similar symptoms. Understanding how insurers may deny claims unfairly can help you recognize problematic tactics.
Billing and coding clues reveal treatment history. Diagnosis codes, physical therapy records, chiropractic visits, and prescription histories create a timeline of prior care.
Prior claims and statements matter significantly. If you filed a workers’ comp claim or previous auto claim involving the same body part, insurers will find it.
Recorded statements can become evidence against you. Adjusters may ask leading questions about when symptoms started or how you felt before the crash. Casual wording gets taken out of context. Trucking companies and their insurers are particularly aggressive with these tactics.
Independent medical exams (IMEs) are evaluations arranged by the insurer. The examining doctor reviews your records and examines you, then writes a report. These reports often dispute causation or minimize the crash’s impact.
Surveillance and social media monitoring can contradict your claimed limitations. Insurers may watch your activity level or review public posts.
Countering Insurers When They Downplay Your Pain
The core insurer theory is simple: they want to show that your pain is actually “same complaints, different day,” rather than “new or worsened condition.” They’ll point to prior pain complaints, old imaging showing degeneration, or gaps in treatment to argue your current problems aren’t new.
When this is the case, it’s important to have thorough and accurate documentation of your condition. This is why we strongly recommend starting pain journal to support your side of the story.
Start with detailing your pre-crash baseline regarding your injury:
- What was your typical pain level (0-10)?
- What medications were you taking?
- Did you have any work restrictions?
- What activities could you do without difficulty?
Then detail how these factors may have changed after your crash:
- Are there new symptoms or pain in new areas?
- Is your pain level higher than before?
- Do you have reduced range of motion?
- Have you missed work or changed job duties?
All of these combined should help you develop the following:
- Timeline: When did symptoms start or worsen relative to the crash?
- Objective findings: What do imaging, exams, and tests show changed?
- Documented functional change: Can you do less now than before the collision?
The key is documenting the differences in your quality of life, not just the history of your pain.
IME Preparation
If you have a pre-existing condition, your insurance company (or the other party’s) might demand that you submit to an independent medical examination. Essentially, this is a third-party evaluation that provides a second opinion on your health and your condition.
However, these are not as “neutral” as they might sound. The examining doctor works for the insurer and writes a report used in your claim. Understand this going in. If you’re scheduled for an independent medical exam, you need to prepare.
- Review your timeline before the appointment
- Be accurate about your pre-crash baseline
- Describe changes clearly and consistently
- Avoid exaggeration or minimization
After the exam, document the appointment length, tests performed, what you reported, and any concerns. Keep these notes for your records.
Imaging Comparisons: How MRI & X-Ray Findings Get Argued
Imaging is often persuasive evidence, but insurers frequently misuse it.
“Degenerative” findings like disc bulges or arthritis are common in adults, even those without symptoms. Insurers argue these findings prove the crash didn’t cause your problems. However, imaging alone can’t prove whether you had pain or limitations before the collision.
When older films exist, radiologists can compare them to post-crash imaging. Look for language in reports describing “interval change” or “new findings.” This comparison language supports aggravation claims.
It’s important to establish a correlation between your accident and your pain using clinical evidence. Documented neurological deficits, range of motion restrictions, and physical exam findings can support imaging arguments even when degenerative changes exist.
Common Insurer Arguments & How to Counter Them
Insurers have a pretty standard playbook when it comes to arguing for pre-existing conditions. Knowing some of the more common tactics they use can help you avoid mistakes that weaken your claim.
“You had it before”: Counter this with documentation showing your baseline function before the crash and measurable changes afterward. Treating physician notes describing the difference are particularly valuable.
“Treatment gap means it’s not serious”: Gaps happen for legitimate reasons. Cost, insurance delays, work obligations, and access issues all cause delays. Document why care was delayed if this applies to you. The Office of Public Insurance Counsel provides guidance on claim processes that may help.
“The MRI shows degeneration”: Reframe the discussion around symptom onset, functional loss, and objective exam changes. Degeneration doesn’t mean you had pain or couldn’t work before the crash.
“You’re back to baseline”: Reaching maximum medical improvement or returning to work doesn’t erase past damages. You may still be entitled to compensation for pain, treatment costs, and lost wages during recovery.
Your Rights in Texas Claim Handling
Texas law provides protections when insurers delay, demand excessive information, or deny claims without clear explanations.
Texas Insurance Code Chapter 541 prohibits unfair settlement practices. Insurers cannot misrepresent policy provisions, fail to acknowledge claims promptly, or refuse to pay claims without conducting reasonable investigations. Request written explanations for any denial.
Texas Insurance Code Chapter 542 establishes prompt payment requirements for certain claims. Tracking deadlines and responses creates a paper trail if disputes arise.
The Texas Department of Insurance rules include a “Bill of Rights” requiring written denial explanations within specific timeframes. You also have the right to refuse requests for information unrelated to your claim.
When to Talk to a Texas Injury Lawyer
Pre-existing conditions don’t automatically defeat claims, but they make proof more technical and insurer pushback more aggressive. If you’re facing stiff resistance from an insurer, it’s a good idea to retain an attorney who can help protect your rights and hold them accountable.
Red flags that suggest you need help:
- Denial or lowball offer citing “pre-existing condition”
- Pressure to sign broad medical authorizations
- IME disputes about causation
- Long delays without explanation
- Blame placed on gaps in your care
An experienced attorney can coordinate record collection, build your timeline, work with treating providers on documentation, arrange expert review when needed, and develop a negotiation strategy.
With over 30 years of experience and more than $1 billion recovered for clients, Angel Reyes & Associates handles these complex cases across Texas. We offer free consultations and charge no fee unless we win. Reach out to us today to discuss your situation.
Pre-Existing Condition FAQs
Can an insurer get my old medical records without my permission after a Texas car accident?
Not usually. Insurers typically need you to sign an authorization, and you can push back on requests that are broader than what is reasonably related to the body parts or conditions at issue.
What if the crash made a previously symptom-free condition start hurting again?
That can still support a valid claim. The key question is whether the collision caused a real change in symptoms, function, or treatment needs, not whether the underlying condition existed on paper before the wreck.
Do I have to turn over records on every prior accident or injury I’ve ever had?
Not always. Prior injuries involving the same body part are usually more relevant than unrelated old conditions, and overdisclosure can give the insurer material to misuse or take out of context.
Can my treating doctor help prove that a crash aggravated a pre-existing injury?
Yes. A treating provider who can describe your condition before the crash, your symptoms after it, and the specific changes in your limitations can be one of the strongest sources of causation evidence.
Can a pre-existing condition affect only the value of my claim instead of defeating it entirely?
Yes. In many cases, the real dispute is not whether you recover anything, but how much of your current pain, treatment, or lost function the insurer attributes to the crash versus your prior condition.







